
Jaundice in newborns is usually harmless and lasts only for a short time, but when you see an adult with yellow skin, it implies a serious health problem that requires urgent medical attention.
Jaundice is a sign of many diseases. There is a yellow discolouration of the skin and sclera (the whites of the eyes) due to excess bilirubin circulating in the body. This is normally accompanied by very dark urine, pale stools (if patients have bile duct obstruction), and other symptoms, such as itchy skin and occasional nausea and loss of appetite.
Excess Bilirubin
Why is there excess bilirubin? Bilirubin is actually a natural 'waste product' arising from the normal breakdown of old red blood cells (RBC) in your body. Under normal circumstances, bilirubin undergoes certain processes in the liver before it is excreted. Bilirubin metabolites are formed in the gut and passed out in the urine and faeces. Bilirubin is also the pigment that gives your urine and faeces colour.
Many reasons can contribute to excess bilirubin in the blood. It is mostly due to problems in the liver or obstruction in the bile ducts, both of which can lead to jaundice. In rare cases, excessive bilirubin is due to haemolytic anaemia, a disorder where an abnormally large number of red blood cells are broken down. 
Common Causes and Symptoms
In general, jaundice can be categorised into 2 types: obstructive jaundice and hepatocellular jaundice.
Obstructive Jaundice
Obstructive jaundice, or cholestatic jaundice, is caused by blockage in the bile ducts due to gallstones, pancreatic cancer, or bile duct cancer (cholangiocarcinoma).
Individuals with obstructive jaundice typically have dark-coloured urine and pale stools because of the reduced flow of bile and bilirubin into the intestines. Pain and fever can be felt if gallstones are present. Because the pain is located at the upper part of the abdomen, patients often misconstrue it as gastric pain.
However, patients with obstructive jaundice due to gallstones usually have upper abdominal pain which radiates to the back. On the other hand, bile duct cancer is usually painless, but can cause weight loss over time.
Obstructive jaundice caused by pancreatic cancer usually presents with pain and weight loss. It is important to pick up pancreatic cancer early and physicians should think about pancreatic cancer, especially when patients present with 'gastric pain'.
Hepatocellular Jaundice
Hepatocellular jaundice is caused by an injury or inflammation of the liver cells. This could be due to:
* Medications (drug-induced jaundice) – Certain prescribed medications or traditional herbal supplements may interfere with liver function. This prevents bilirubin from being efficiently removed from the blood or excreted into the bile, thus leading to jaundice.
* Viral hepatitis – Hepatitis is a condition where the liver becomes inflamed and its ability to process and secrete bilirubin is largely discounted. Common forms of viral hepatitis include viral hepatitis A, B, and C. Viral hepatitis A is normally contracted through shell fish whereas viral hepatitis B and C are through blood products and body fluids. Alcohol hepatitis is another important cause of hepatocellular jaundice.
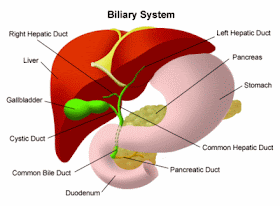 * Chronic liver diseases – In chronic liver diseases (e.g. chronic hepatitis B, alcoholic liver disease), scar tissue can form in the liver. Scar tissue cannot do what healthy liver tissue does. As more scar tissue replaces the normal functioning liver tissue, the liver function deteriorates (e.g. unable to clean blood, digest food, and store energy).
* Chronic liver diseases – In chronic liver diseases (e.g. chronic hepatitis B, alcoholic liver disease), scar tissue can form in the liver. Scar tissue cannot do what healthy liver tissue does. As more scar tissue replaces the normal functioning liver tissue, the liver function deteriorates (e.g. unable to clean blood, digest food, and store energy).
Ultimately, there will be jaundice. By the time jaundice is noticeable, the condition may have already become serious, and patients may experience liver failure and complications of liver cirrhosis (hardening of liver).
Finding Out What’s Wrong
It is important for the doctor to determine the underlying health conditions leading to the jaundice so that appropriate treatment can be given to the patient. The jaundice usually resolves once the underlying cause is treated.
History and physical examination can suggest possible reasons for the jaundice. For instance, jaundice is most likely caused by alcoholic liver disease if the patient is a heavy drinker, or may be drug-induced if patient is taking new medications recently.
 Presence of abdominal pain and fever may suggest blockage of the bile duct, usually by gallstones. If there is weight loss, it could be cancer related.
Presence of abdominal pain and fever may suggest blockage of the bile duct, usually by gallstones. If there is weight loss, it could be cancer related.
Liver function tests for measuring bilirubin and liver enzymes are helpful to determine if the jaundice is due to abnormal RBC destruction, inflammation of the liver, or obstruction or disease in the bile duct. A liver function test can help suggest what is the probable cause of jaundice. Blood tests can be done to test for hepatitis A, B, and C.
An ultrasound scan of the abdomen may help to detect obstructions in bile ducts, e.g. gallstones or pancreatic cancer.
Computerised tomography (CT) scans and MRI scans are especially useful to identify tumours in the pancreas and liver. It is also useful to detect bile duct tumour.
Endoscopic ultrasound is particularly useful to examine the pancreas for tumours or small gallstones in the gallbladder and bile ducts that cannot be detected by other methods. It is also useful to take some tissues using fine needle aspiration.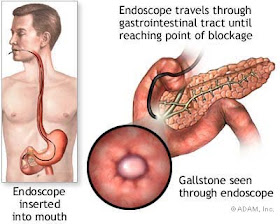 Treatment
Treatment
Before a doctor treats a jaundiced patient, he has to find out the cause first, so that treatment may be directed at the specific cause. For example, hepatitis B is treated with anti-viral drugs, while a procedure called Endoscopic Retrograde Cholangiopancreatography (ERCP) is performed to remove a gallstone in the bile duct or to insert a stent in the bile duct to unblock the blockage in the bile duct due to tumour.
If the jaundice is associated with alcoholic hepatitis, the patient has to stop alcohol intake.
The main treatment for bile duct cancer is surgery to remove the tumour, but operation is not always possible. When that’s the case, a small tube (stent) will be put into the bile duct to allow the bile to flow again and relieve the jaundice.

Prevention
Jaundice can be prevented if your liver is healthy and functioning efficiently. While causes such as pancreatic cancer and bile duct cancer cannot be prevented, there are things you can do to protect your liver.
* Avoid excessive intake of alcohol.
* If you have not had hepatitis A or B, get vaccinated.
* There is no vaccine available for hepatitis C, but you can reduce your risk by practising safe sex and avoiding injecting drugs or sharing intravenous drug needles. All the needles in hospitals nowadays are single-use.
* Make sure shellfish are cooked properly before eating to prevent hepatitis A.
* For people with gallstones, eating a low-fat diet helps to reduce the attack of pain. If the gallstones give you symptoms, remove it.
As with most diseases, timely and appropriate treatment saves lives, so seek medical help as soon as you notice any signs of jaundice, or experience intense abdominal pain and fever.
by Dr Tan Huck Joo

0 Komentar untuk "Jaundice - The Yellow Symptom"